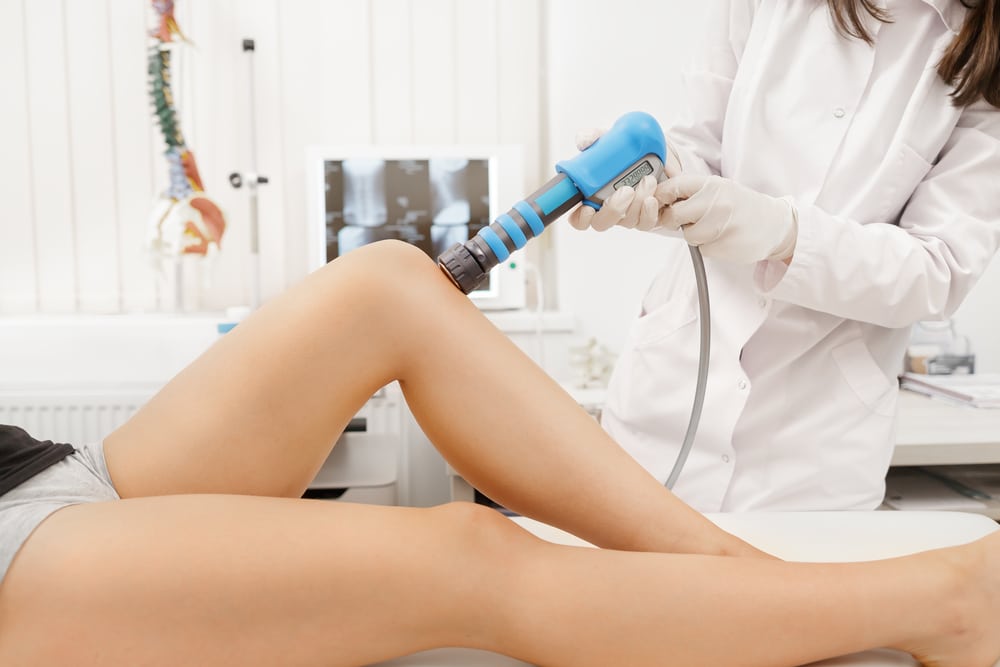
Shockwave Therapy for Knee Pain: A Revolutionary Treatment by Your Trusted Chiropractor in Hollywood, Florida
Knee pain is a common complaint, affecting millions of people worldwide. Whether it’s due to arthritis, sports injuries, or overuse, knee pain can significantly impact your quality of life. Traditional treatments like physical therapy, medications, or even surgery have their place, but there’s a newer, non-invasive option that’s gaining popularity: shockwave therapy. If you’re in Hollywood, Florida, and seeking relief from knee pain, a sports chiropractor might offer the solution you need.
What is Shockwave Therapy?
Shockwave therapy is a non-invasive treatment that uses high-energy sound waves to stimulate healing in damaged tissues. Originally developed to treat kidney stones, this technology has since been adapted to address a variety of musculoskeletal conditions, including knee pain. If you’re in Hollywood, Florida, and dealing with knee pain, visiting a sports chiropractor who offers shockwave therapy could be a game-changer.
The treatment works by delivering acoustic waves to the targeted area. These waves promote blood flow, reduce inflammation, and accelerate the body’s natural healing process. Shockwave therapy is particularly effective in treating conditions like patellar tendinitis (jumper’s knee), osteoarthritis, and chronic knee pain that hasn’t responded well to other treatments.
How Does Shockwave Therapy Work?
During a shockwave therapy session, a handheld device is used to deliver high-energy sound waves to the knee. The procedure typically takes about 15 to 20 minutes, and most patients require several sessions spaced over a few weeks for optimal results. At Miami Spine and Performance, our sports chiropractor can guide you through this treatment to ensure the best outcome.
The sound waves penetrate the skin and reach the injured tissue, where they:
1. Increase Blood Flow: The increased circulation helps bring nutrients and oxygen to the damaged area, promoting faster healing.
2. Reduce Inflammation: Shockwave therapy can help reduce the inflammation that often accompanies chronic knee pain, providing relief from pain and swelling.
3. Stimulate Collagen Production: Collagen is a key component of healthy tendons and ligaments. By stimulating its production, shockwave therapy helps strengthen these tissues, improving joint stability.
4. Break Down Scar Tissue: The acoustic waves can help break down fibrous scar tissue, which can restrict movement and contribute to pain.
Benefits of Shockwave Therapy for Knee Pain
Shockwave therapy offers several advantages over traditional treatments:
– Non-invasive: Unlike surgery, there are no incisions or downtime, and the risk of complications is minimal.
– No Medications: Shockwave therapy is drug-free, making it a suitable option for those who prefer to avoid medications.
– Quick Recovery: Most patients experience little to no downtime and can return to their normal activities quickly.
– Effective for Chronic Conditions: Many patients with chronic knee pain that hasn’t responded to other treatments have found relief with shockwave therapy.
Is Shockwave Therapy Right for You?
While shockwave therapy is effective for many types of knee pain, it’s not suitable for everyone. It’s most effective for chronic conditions, particularly those involving tendons, ligaments, and soft tissues. Patients with acute injuries, blood clotting disorders, or certain types of nerve pain may not be ideal candidates. Consulting with a sports chiropractor in Hollywood, Florida, can help you determine if this treatment is right for you.
Before starting treatment, a thorough evaluation by a healthcare professional is essential to determine if shockwave therapy is the right choice for your knee pain.
What to Expect During Treatment
Shockwave therapy sessions are typically well-tolerated, but you may feel some discomfort during the procedure, especially if the treatment area is highly sensitive. The intensity of the treatment can be adjusted based on your comfort level.
After the session, you may experience mild soreness or swelling, similar to what you might feel after a vigorous workout. This is a normal part of the healing process and should subside within a few days.
Most patients begin to notice improvement after the first few sessions, with continued progress over the following weeks as the body heals.
Shockwave therapy is an innovative and effective treatment for knee pain, offering a non-invasive alternative for those who haven’t found relief through other methods. By stimulating the body’s natural healing processes, shockwave therapy can help you get back to the activities you love, pain-free.
If you’re struggling with knee pain in Hollywood, Florida, and are interested in exploring shockwave therapy, consult with a local sports chiropractor to see if this treatment is right for you. With its minimal risks and potential for significant relief, shockwave therapy might just be the solution you’ve been looking for. Visit a trusted chiropractor in Hollywood, Florida today to learn more about how shockwave therapy can help you regain your mobility and live pain-free.

